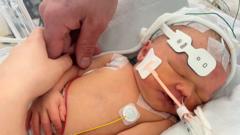
When a newborn turns purple, the clock does not just tick; it screams. This phenomenon, often clinically referred to as cyanosis, is the physical manifestation of a body starved of oxygen. For many parents, the sight of their infant’s skin darkening into a bruised, dusky plum is the first and only warning that something has gone catastrophically wrong with the heart or lungs. However, the true crisis lies not just in the biological failure of the infant, but in a systemic failure of detection that begins long before the baby leaves the hospital.
The core issue remains a dangerous reliance on visual assessment and the inconsistent application of pulse oximetry screening. While modern medicine prides itself on precision, the identification of "the purple baby" often falls to the subjective observation of exhausted parents or overstretched nursing staff. This gap in the safety net means that Critical Congenital Heart Disease (CCHD) or respiratory distress can go unnoticed until the infant is in the throes of a life-threatening "spell." We are treating the symptom when we should be perfecting the surveillance.
The Biology of the Blue Baby
To understand why a baby turns purple, one must look at the mechanics of hemoglobin. Oxygenated blood is bright red. Deoxygenated blood is darker, appearing blue or purple when viewed through the translucent skin of a neonate. When the arterial oxygen saturation drops below 85%, the visual change becomes apparent to the naked eye.
But here is the catch. By the time a parent notices their child is purple, the infant may have been struggling for hours. Central cyanosis—bluish discoloration of the tongue and mucous membranes—is a late-stage indicator. Peripheral cyanosis, or acrocyanosis, is common in the first 24 hours of life and is often benign. Distinguishing between a cold baby and a dying baby requires more than a casual glance. It requires data.
The heart is essentially a pump with a complex electrical and structural blueprint. In cases of CCHD, such as Transposition of the Great Arteries or Tetralogy of Fallot, the "plumbing" is wired incorrectly. Blood bypasses the lungs, recirculating through the body without picking up fresh oxygen. These infants are often born appearing healthy because they are supported by the ductus arteriosus, a temporary fetal blood vessel. Once that vessel closes—usually within days of birth—the baby’s oxygen levels plummet. If the baby is already at home, the purple hue is a sign that the window for a safe intervention is closing.
The Screening Deficit
Despite universal recommendations, the implementation of pulse oximetry remains uneven. This simple, non-invasive test measures the percentage of hemoglobin saturated with oxygen. It is the only reliable way to catch "silent" hypoxia before the physical purple transition occurs.
A standard screen involves placing a sensor on the right hand and either foot. A passing result is a saturation of 95% or higher in both extremities, with less than a 3% difference between them. If a baby fails this screen, it triggers an immediate echocardiogram.
The problem is the "gray zone." Many hospitals perform the screen at 24 hours of age, but some infants are discharged earlier. Others may have borderline results that are dismissed as "adjustment issues." When these babies go home, parents are told to watch for "difficulty breathing" or "color changes." This puts the burden of medical diagnosis on a layperson who has likely never seen a cyanotic infant. A parent is not a pulse oximeter. They cannot be expected to differentiate between a crying jag and a cardiac emergency.
Beyond the Heart
While cardiac issues are the most feared cause of the purple baby, they are not the only culprits. Sepsis, the silent killer of neonates, can cause rapid respiratory failure and subsequent cyanosis. When an infection takes hold, the body’s metabolic demands skyrocket, and the lungs cannot keep pace.
Methemoglobinemia is another, rarer factor. This occurs when the iron in the blood is oxidized, preventing it from carrying oxygen. These babies are often described as "chocolate-colored" or deep purple, yet they may not appear to be in respiratory distress initially. This complicates the clinical picture. A doctor looking for gasping breaths might miss a baby whose blood is simply chemically incapable of doing its job.
Then there is the issue of skin tone. Visual assessment for cyanosis is inherently biased toward lighter skin. In infants with higher melanin levels, the purple or blue tint is much harder to detect. This is a fundamental flaw in traditional pediatric training that emphasizes "turning blue" as a primary warning sign. If the medical community continues to rely on visual cues, it will continue to fail infants of color at a disproportionate rate.
The Cost of Silence
The financial and emotional toll of a missed diagnosis is staggering. An infant who arrives at an Emergency Room in a "cyanotic spell" requires intensive, high-cost stabilization. This often includes intubation, prostaglandin infusions to reopen fetal pathways, and emergency transport to a level IV NICU.
In contrast, a baby identified through routine, rigorous screening can be managed in a controlled environment. The surgery is planned, the family is prepared, and the risk of neurological damage from prolonged hypoxia is significantly reduced. We are spending millions on reactive crisis management because we refuse to mandate a foolproof proactive standard.
Professional Fatigue and Parental Intuition
We must address the human element. Healthcare workers are operating in a state of chronic burnout. A nurse checking twenty babies in a shift might glance at a sleeping infant and see "resting comfortably" rather than "lethargic and hypoxic."
Parental intuition is often the final line of defense, yet it is frequently patronized. When a mother says, "I knew something was wrong," she is usually reacting to a cluster of subtle signs: a weak suck during feeding, a peculiar coolness of the hands, or a tint to the lips that wasn't there four hours ago. Medical professionals must stop viewing parental concern as "anxiety" and start viewing it as a valid clinical observation.
The False Security of the "Normal" Discharge
The most dangerous moment in a newborn’s life is the transition from the hospital to the car seat. The "all-clear" given at discharge creates a false sense of security. Parents assume that if their baby were sick, the experts would have caught it.
However, the closing of the ductus arteriosus is a biological event that follows its own timeline, not a hospital’s discharge schedule. A baby can pass every test at 24 hours and be in full cardiac collapse at 72 hours. Education must shift. We need to stop telling parents that "purple is bad" and start teaching them that "any change in vigor or color" requires an immediate return to the hospital.
A Mandatory Standard for Survival
The solution is not more pamphlets or "awareness" campaigns. It is the aggressive, standardized application of technology.
- Universal Pulse Oximetry: This must be a hard requirement for discharge, regardless of the birth setting, including home births and birthing centers.
- Post-Discharge Follow-up: A mandatory 48-hour check-up specifically focused on cardiac and respiratory stability, not just weight gain.
- Home-Based Monitoring for At-Risk Groups: Infants with borderline screening results should be sent home with medical-grade oximeters, not just "watchful waiting" instructions.
- Bias Correction in Training: Medical education must move away from "blue" as a benchmark and toward oxygen saturation numbers and mucosal membrane checks that apply to all ethnicities.
We cannot continue to rely on the hope that a parent will notice their child’s skin changing color in the middle of the night. Hope is not a medical protocol. The technology to prevent these tragedies exists, is inexpensive, and is easily deployed. Every instance of a baby turning purple at home represents a failure of the system to do its job before the family left the building.
The focus must move from the dramatic rescue of the "purple baby" to the quiet, data-driven prevention of the crisis itself. When the skin changes color, the battle is already halfway lost. We must win the fight while the baby is still pink.
Standardize the screening. Trust the data. Listen to the parents. Stop the clock before the screaming starts.